Translate this page into:
Aplasia cutis congenita of scalp
-
Received: ,
Accepted: ,
How to cite this article: Selvam O, Singh Y, Kuruvila S. Aplasia cutis congenita of scalp. South Asian J Health Sci. 2024;1:51–2. doi: 10.25259/SAJHS_19_2023
A five-hour-old male child presented to us with reddish lesions over the scalp from birth. There was no history of any trauma during birth or of instrumental delivery. There was neither a history of similar lesions elsewhere in the body nor history of similar complaints in the family. Cutaneous examination revealed a single reddish ulcer with a well-defined margin and granulomatous floor of size measuring approximately 1 × 1 cm over the vertex of the scalp with no underlying skull defect [Figure 1]. There were no other associated anomalies. A clinical diagnosis of Aplasia cutis congenita, Frieden’s type I was made, and parents were reassured.
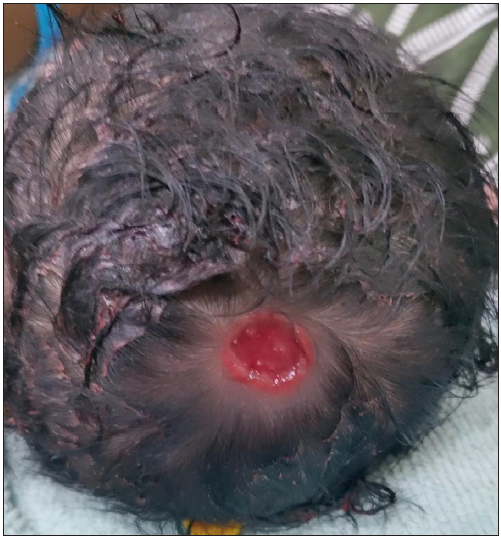
- A single reddish ulcer with well defined margin and granulomatous floor of size measuring approximately 1 × 1 cm over the vertex of scalp.
Aplasia cutis congenita (ACC) is a rare malformation with an incidence of 1:12,000, sporadic in nature, characterised by localised congenital absence of the skin.[1] ACC often presents as a solitary lesion involving the scalp but can also involve other parts of the body. ACC located at the vertex can be due to the maximum tensile force during accelerated brain growth or in that region, which occurs during Weeks 10–15 of gestation.[2] A hair collar sign characterised by a collarette of dark, coarse hair around the lesion can be an indicator of an underlying neural tube defect.[3] Type 1 ACC may be associated with cleft lip and/or palate, tracheoesophageal fistula, patent ductus arteriosus, intestinal lymphangiectasia, omphalocele, polycystic kidneys, and double cervix and uterus. Treatment predominantly involves conservative management and topical antibiotics where required. Early surgical correction is recommended for larger lesions and underlying defects. The prognosis of Frieden’s type l ACC is excellent as the lesion heals spontaneously as a hairless smooth scar in approximately 28 days, few as atrophic scars and rarely as hypertrophic scars.[1] ACC is diagnosed clinically, and biopsies are provisionally not performed. Dermatologists and neonatologists are cognisant of the condition to rule out any underlying defects that need timely intervention.
Ethical approval
The Institutional Review Board approval is not required.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
Dr. Sheela Kuruvila is on the Editorial Board of the Journal.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
References
- Abdominal aplasia cutis congenita with fetus papyraceus: Frieden’s class V. Indian J Paediatr Dermatol. 2023;24:54-6.
- [Google Scholar]
- Aplasia cutis congenita of the scalp—What are the steps to be followed? Case report and review of the literature. An Bras Dermatol. 2015;90:100-3.
- [CrossRef] [PubMed] [Google Scholar]
- Bullous variant of aplasia cutis congenita: A rare entity. Indian J Paediatr Dermatol. 2022;23:179-80.
- [Google Scholar]